Select Language:
Millions of people worldwide take medication daily to manage high blood pressure, also known as hypertension. It’s one of the most prevalent health issues, especially among older adults. If left untreated, hypertension can increase the risk of heart attacks, strokes, kidney disease, and other severe health problems. To help reduce these risks, doctors often prescribe medications to lower blood pressure and safeguard long-term health.
One common class of these medications is called Calcium Channel Blockers, or CCBs. These drugs work by relaxing and widening blood vessels, making it easier for blood to flow throughout the body. Examples like amlodipine and nifedipine are widely used and generally safe for long-term use, playing a crucial role in hypertension treatment.
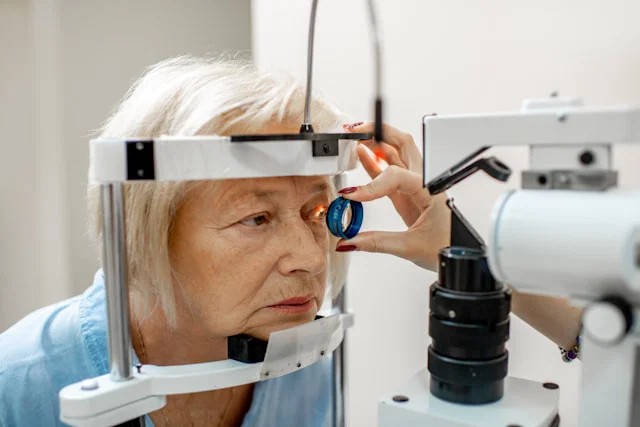
However, recent research indicates a possible link between Calcium Channel Blockers and an eye condition known as glaucoma. This serious eye disease gradually damages the optic nerve, which is vital for transmitting visual signals to the brain. If glaucoma isn’t treated, it can lead to permanent vision loss. The study, led by Dr. Alan Kastner from Moorfields Eye Hospital and University College London, examined health records from over 427,000 adults in the UK. Around 33,000 of these individuals were taking Calcium Channel Blockers.
Results showed that people using these medications had a higher chance of being diagnosed with glaucoma compared to those not on these drugs. Notably, this increased risk persisted even after accounting for factors like age, smoking, lifestyle habits, and other health conditions. Interestingly, this connection was specific to Calcium Channel Blockers; other types of blood pressure medications did not show the same association with glaucoma.
Glaucoma primarily harms the optic nerve, slowly deteriorating vision over many years. Often, symptoms are unnoticed until significant and irreversible vision loss occurs, earning it the nickname “the silent thief of sight.” While elevated eye pressure has long been considered a leading cause of glaucoma, this new research suggests that people on Calcium Channel Blockers may develop early signs of the disease even when their eye pressure appears normal. This hints at other possible mechanisms, such as alterations in blood flow or impacts on inner eye structures, though more studies are needed to understand these effects.
The findings highlight how both hypertension and glaucoma can develop quietly without obvious symptoms. Regular medical check-ups and eye exams are critical, especially for older adults and those with other risk factors like a family history or diabetes. Experts caution against stopping prescribed blood pressure medications abruptly, as uncontrolled hypertension poses significant health dangers. Instead, patients are advised to consult their physicians about these findings and consider routine eye screenings, particularly if they belong to higher-risk groups.
Early detection of glaucoma allows for treatments that can slow or stop vision loss, reinforcing the importance of routine eye exams, optic nerve assessments, and intraocular pressure measurements. While the study presents important insights, further research is necessary to confirm the connection, particularly since some authors have ties to pharmaceutical companies. Independent studies will be essential in verifying these findings and guiding clinical practice.
Ultimately, this research underscores how medications targeting one part of the body can sometimes produce unexpected effects elsewhere. As scientists learn more about the relationship between blood pressure medications and eye health, future treatments may become safer and more personalized.
For individuals concerned about hypertension, exploring lifestyle changes—such as reducing unhealthy habits—and drinking green tea might help manage blood pressure levels. Additionally, understanding what foods to eat or avoid to control high blood pressure, along with incorporating blood pressure-lowering foods, can be beneficial.
This study was published in the journal JAMA Ophthalmology.
Copyright © 2026 Knowridge Science Report. All rights reserved.