Select Language:
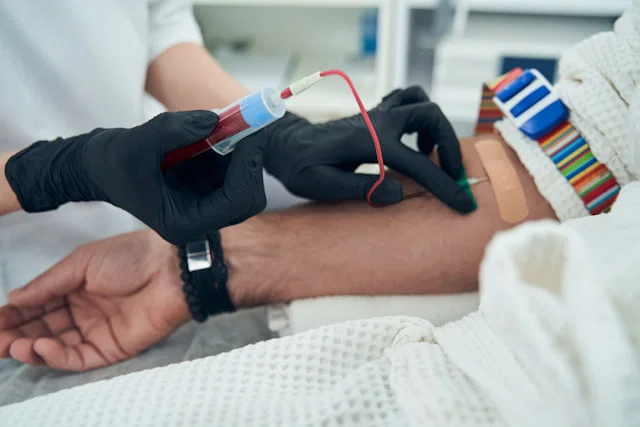
Testicular cancer ranks among the most common types of cancer in young men, particularly teenagers as well as those in their twenties and thirties. The encouraging news is that if detected early, many cases can be successfully treated. However, catching it in its early stages isn’t always straightforward. Some tumors don’t produce clear signs on standard blood tests, which can sometimes delay diagnosis and treatment.
Researchers at the Mayo Clinic have recently developed a new method to identify testicular cancer with a simple blood test. Their study, published in Nature Communications, introduces a technique that examines the immune system’s signals rather than relying solely on traditional tumor markers.
Typically, doctors look for specific substances produced by tumors—called tumor markers—via blood tests. But not every testicular cancer produces enough of these markers to be detected easily. Consequently, some patients may have cancer even when their test results appear normal, making diagnosis more complicated and stressful.
To overcome this, scientists used an innovative approach. Instead of tracking just a few markers, they analyzed thousands of immune system signals simultaneously. The immune system reacts in complex ways to cancer, and these responses can leave distinctive patterns in the blood.
Using this strategy, they developed a test called GCT-iSIGN. Their analysis of 427 blood samples showed promising results: the test correctly identified 93% of individuals with germ cell tumors and accurately ruled out cancer in 99% of those without the disease. Remarkably, it detected 23 out of 24 cancers that standard blood tests had missed, suggesting this method could help uncover cancers that might otherwise go unnoticed.
The researchers also created another test, Sem-iSIGN, which helps distinguish between the two primary types of testicular cancer. This distinction is crucial since each type may require a different treatment approach. Early identification of the specific cancer type can enable more tailored and effective treatments.
This research builds on earlier work by the same team, where they used similar immune-based methods to identify markers linked to rare neurological conditions associated with cancer. These previous discoveries laid the groundwork for developing the current tests.
Dr. Divyanshu Dubey, the lead researcher, explained that when traditional blood tests fail to provide clear answers, diagnosis can be significantly delayed. Such delays can impact treatment outcomes. The new, more sensitive test could potentially improve early detection and, ultimately, patient care.
Nonetheless, it’s important to note that this research is still in the early stages. Further studies involving larger patient groups are necessary to confirm the effectiveness and reliability of these tests before they become routine in clinical settings.
Overall, this breakthrough represents an exciting advancement in cancer detection technology. It highlights the potential for immune system analysis to uncover diseases that are difficult to find with conventional methods. If future research validates these findings, this blood test might become a vital tool for early cancer detection, especially among young men.
While the results are promising, caution is warranted. The current study involved a limited sample size, so additional research will be essential to confirm accuracy and effectiveness. However, with its high detection rates and ability to identify cases missed by standard testing, this approach shows considerable promise. If proven effective, it could lead to quicker diagnoses, earlier treatments, and better outcomes for many patients.
Those interested in cancer research should also consider studies suggesting that a low-carb diet might increase overall cancer risk, whereas vitamin D supplements could substantially reduce the risk of death related to cancer. Other recent findings indicate that drinking milk may influence the risk of heart disease and cancer, and higher consumption of dairy foods has been linked to an increased risk of prostate cancer.
Source: Mayo Clinic.