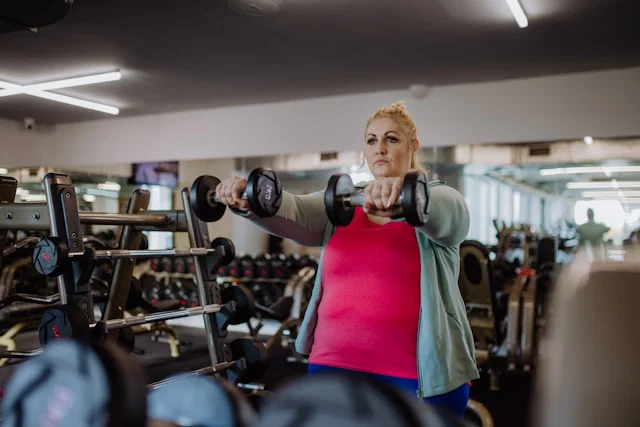Select Language:
A new study indicates that both weight loss medications and bariatric surgery can significantly improve body composition in individuals with obesity. The research, conducted by Vanderbilt Health and published in JAMA Network Open, demonstrates that these treatments help decrease body fat while only minimally reducing lean body mass, such as muscle tissue. Maintaining a proper balance between fat and muscle is crucial for long-term health benefits.
Obesity remains a rising health concern worldwide, associated with increased risks of heart disease, diabetes, and certain types of cancer. For individuals affected, losing weight can lead to notable health improvements.
However, not all weight loss offers the same benefits. Losing fat is advantageous, but excessive muscle loss can be detrimental since muscle supports movement, strength, and boosts metabolism. Additionally, maintaining muscle mass has been linked to a lower risk of mortality.
The researchers aimed to evaluate how different obesity treatments influence fat mass and fat-free mass over time. Fat mass refers to the body’s fat content, while fat-free mass includes muscles, bones, and other tissues. Higher proportions of fat are associated with greater health risks, whereas a higher ratio of fat-free mass tends to be linked to increased survival rates.
Data from over 3,000 patients formed the basis of the analysis. Some of these patients had bariatric surgery between 2017 and 2022, while others were treated with newer GLP-1 receptor agonist medications—such as semaglutide and tirzepatide—between 2018 and 2023. These drugs work by suppressing appetite and promoting satiation to aid weight loss.
The study populations were selected to include adults aged 18 to 65, excluding individuals with certain severe health issues to ensure more precise results. Researchers used bioelectrical impedance analysis—a technique estimating body composition based on electrical conductivity, which takes into account factors like height, weight, age, and medical history.
Over a span of two years, both groups exhibited similar patterns: significant fat reduction accompanied by only a slight decrease in fat-free mass. This resulted in an overall favorable change in body composition, with a healthier balance of muscle to fat.
Gender differences also emerged. Men tended to retain more muscle mass during weight loss, while women experienced marginally higher losses in lean tissue. These findings suggest that sex may influence how body composition responds to treatment.
The results emphasize that effective obesity management should focus not solely on weight loss but also on preserving muscle tissue for overall health. Simply reducing weight isn’t enough; the quality of weight lost is equally important.
The study has some limitations, as it was based on real-world health records rather than controlled clinical trials, which reduces the ability to establish cause-and-effect relationships. Additionally, the body composition measurement method used provides estimates rather than exact figures.
In summary, both surgical and pharmaceutical interventions can enhance body composition, but attention must be paid to muscle preservation. Future research could explore combining these treatments with targeted exercise and nutrition strategies to optimize lean mass retention.
Ultimately, this study underscores that improving body composition—reducing fat while maintaining or increasing muscle—is key to long-term health. More personalized approaches are necessary to maximize treatment benefits and patient outcomes.