Select Language:
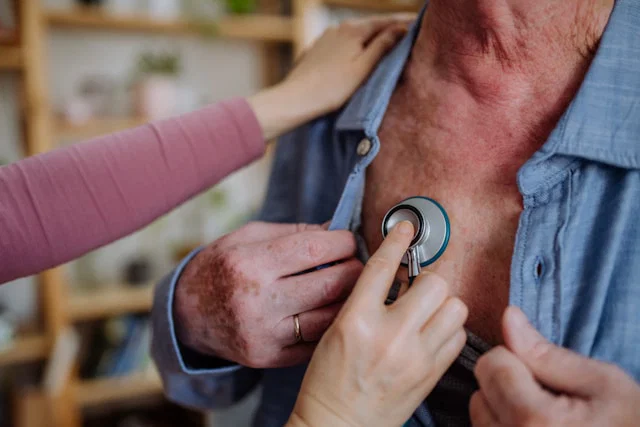
When people hear the term “heart attack,” their first thought often goes to clogged arteries. This is the most common reason—fatty deposits block blood flow to the heart. But not every heart attack occurs this way.
Some individuals experience heart attack symptoms along with abnormal blood tests, yet their arteries appear normal on scans. This condition is known as myocardial infarction with non-obstructive coronary arteries, or MINOCA.
For years, MINOCA has puzzled both healthcare providers and patients. People might have intense chest pain and be diagnosed with a heart attack, but standard tests can’t pinpoint the cause. This uncertainty can be unsettling, especially for younger patients or women, who often don’t fit the typical profile of heart disease.
A groundbreaking study led by researchers at NYU Grossman School of Medicine brings new insights. Published in the journal Circulation, the research demonstrates that using two advanced imaging techniques together can identify the underlying cause of these heart attacks in most cases.
This is one of the largest studies of its kind, involving 336 patients from 28 hospitals across the U.S., Canada, and the U.K. The average age was 58, with most participants being women—reflecting the higher prevalence of MINOCA among women.
To investigate what was happening inside these patients’ arteries, doctors employed two imaging methods. The first is called optical coherence tomography (OCT). This involves inserting a tiny device into the arteries to obtain highly detailed images of the arterial walls. It can reveal subtle issues like small tears or tiny blood clots that standard scans might miss.
The second method is cardiac magnetic resonance imaging (MRI), which produces clear pictures of the heart muscle. This technique helps identify damage and determine whether it stemmed from inadequate blood flow, inflammation, or other factors.
When combined, these tests provided remarkably definitive results. Doctors could determine the probable cause of the heart problem in 79% of patients—significantly better than traditional approaches.
The study revealed that about 59% of the patients truly experienced a heart attack caused by decreased blood flow, possibly due to tiny plaques, spasms in the arteries, or small clots. Another 20% had conditions that mimic heart attacks but are caused by different issues, such as myocarditis (inflammation of the heart muscle) or stress-induced conditions like Takotsubo syndrome.
Differentiating these causes is crucial because they demand different treatments. Without precise diagnosis, patients might not get the care they need or could receive ineffective treatments.
Importantly, the findings suggest that relying solely on symptoms or basic tests isn’t enough to determine who needs advanced imaging. Even patients with mild symptoms may have significant heart damage, making the use of both imaging techniques essential in many cases.
Presented at the American College of Cardiology’s Annual Scientific Session and published in Circulation, these findings carry substantial implications for healthcare. They validate current guidelines that recommend additional imaging workups and underscore the limitations of standard diagnostic tools, which can miss important details.
However, there are challenges. These advanced imaging methods require specialized equipment and trained professionals, which might not be available in all hospitals. More research is needed to make these techniques more accessible and to develop tailored treatment plans based on the specific causes identified.
Overall, this study marks a significant advance, revealing that heart attacks can be more complex than previously understood. Better diagnostic tools mean more accurate diagnoses and more effective care.
If you’re interested in health topics, consider reading about the potential benefits of low-dose lithium supplements or exploring what current research says about egg consumption and heart health. Additional studies also offer insights on potatoes and high blood pressure, along with the best types of bread for people with heart disease.
Source: NYU Grossman School of Medicine.