Select Language:
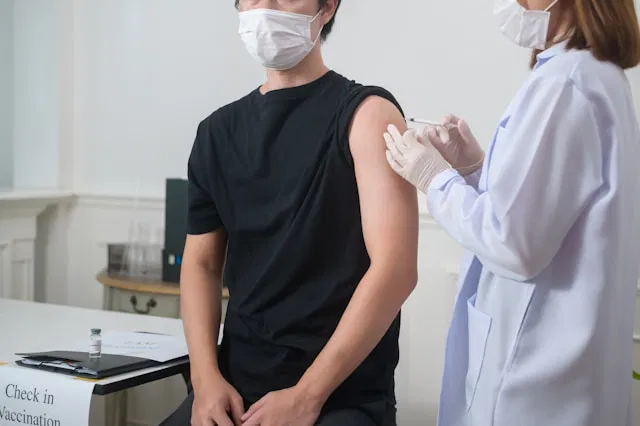
Many people view the flu as a seasonal illness characterized mainly by fever, cough, and fatigue. However, recent research indicates that influenza can pose much more serious risks to the body. A new study published in Eurosurveillance reveals that getting the flu significantly elevates the chances of experiencing a heart attack or stroke—an increased risk that vaccination may help mitigate, even if infection still occurs.
When the body battles the flu virus, it triggers a robust immune response, which often leads to widespread inflammation. While inflammation is a natural part of fighting infection, it can also weaken blood vessel stability and promote blood clot formation. These changes can spark critical events like heart attacks and strokes, particularly among older adults or individuals with pre-existing health conditions.
The study, led by Croci and colleagues, focused on understanding how substantial this risk is and whether receiving the flu vaccine can provide ongoing protection after infection. Using detailed health records from Denmark—where each individual has a unique ID that links various medical data—they analyzed the health outcomes of 1,221 adults aged 40 and older who experienced their first hospital admission for a heart attack or stroke following a confirmed flu infection. The data spanned nine flu seasons from 2014 to 2023, examining the timing of infections, vaccination status, and subsequent cardiovascular events.
Findings revealed a pronounced pattern: the week immediately following a flu infection posed the highest danger. During this period, the likelihood of stroke tripled, and the chance of a heart attack increased fivefold, compared to other times. This suggests that catching the flu can act as a trigger for these severe cardiovascular incidents.
Importantly, vaccination proved to cut this risk considerably. Those who had received a flu shot experienced about a 50% reduction in the heightened danger. This indicates that even if the vaccine does not prevent infection entirely, it still offers protection against serious complications.
The researchers employed a study design that compares each individual’s risk at different time points, minimizing confounding factors such as lifestyle or chronic health issues. This approach enhances the credibility of the results. However, the study had some limitations—such as not evaluating different vaccine types or the effectiveness of yearly vaccine matching to circulating strains. Additionally, variables like gender or the timing of vaccination weren’t specifically analyzed, and differences in healthcare systems across countries could influence generalizability.
Despite these limitations, the findings emphasize an important message: the flu vaccine may do more than prevent the illness itself. It appears to reduce the likelihood of life-threatening complications like heart attacks and strokes, even in cases where infection occurs. This broadens the perspective on vaccination as a vital component of overall health protection, especially for older populations.
These insights could bolster public health initiatives aimed at increasing vaccination rates, helping to lower both flu transmission and the incidence of cardiovascular events. Furthermore, the evidence underscores the economic and societal benefits of vaccination programs, as preventing severe health events can lead to decreased healthcare costs and improved quality of life.
In conclusion, influenza’s risks extend beyond respiratory symptoms, including hidden dangers to heart and brain health. While further research is necessary, current data strongly suggest that a flu shot can save lives—not just by staving off the flu, but by safeguarding against potentially fatal heart and brain conditions during vulnerable periods.